Munenori Uemura, PhD1, Noriyuki Matsuoka2, Morimasa Tomikawa, MD, PhD, FACS1, Makoto Hashizume, MD, PhD, FACS1, Yousuke Seki, MD, PhD3, Yoshimochi Kurokawa, MD, PhD3. 1Kyushu University, Japan, 2Kyoto Kagaku Company, Japan, 3Yotsuya Medical Cube, Japan
INTRODUCTION: The purpose of this study was to evaluate the validity of a newly developed system for assessing suturing skills in laparoscopic surgery (Fig. 1).
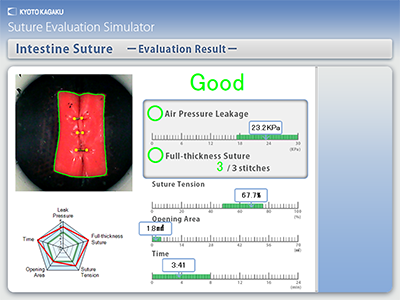
METHODS AND PROCEDURES: Fig. 1 shows our newly-developed computerized system for objective assessment of suturing skills by using a laparoscopic intestinal suturing model, E-Lap. The system includes a new artificial intestinal model that mimics living tissue and pressure-measuring and image-processing devices. Each examinee performs a specific skill using the artificial model, which is linked to a Suture Simulator Instruction Evaluation Unit. The model uses internal air pressure measurements and image processing to evaluate suturing skills. Five criteria, scored on a five-grade scale, were used to evaluate participants’ skills (Fig. 2). The volume of air pressure leak was determined by the volume of air inside the sutured artificial intestine. For example, for the criterion “air pressure leakage”, the approximate midpoint of the acceptable range was Grade 3. Values lower than the minimum acceptable value received lower grades and those above the midpoint of the acceptable range higher grades.
We enrolled 152 surgeons who attended a laparoscopic surgery training course (Series 150–156, March to July, 2016) held by the Japan Society for Endoscopic Surgery (JSES). Participants performed the skill assessment suturing task using the E-Lap pre- and post-training and the resultant pairs of scores were compared.
RESULTS: The pre- and post-course scores for air pressure leak were 1.36 ± 1.35 and 1.78 ± 1.20, respectively; for full-thickness sutures 3.57 ± 1.53 and 4.21 ± 1.03, respectively; for suture tension 2.99 ± 1.24 and 3.13 ± 1.18, respectively; for area of wound opening 4.03 ± 1.14 and 4.28 ± 0.94, respectively; and for performance time 2.45 ± 0.87 and 3.15 ± 0.96, respectively. Significant differences (p < 0.01) between pre- and post-course scores were observed for all criteria except suture tension.
CONCLUSIONS: This system has sufficient validity for quantitative assessment of suturing skill in laparoscopic surgery and is therefore a useful tool for training and assessment of laparoscopic surgeons.

Presented at the SAGES 2017 Annual Meeting in Houston, TX.
Abstract ID: 79100
Program Number: P309
Presentation Session: Poster (Non CME)
Presentation Type: Poster
