Satoshi Ieiri, MD, PhD1, Satoshi Obata, MD1, Takahiro Jinbo, MD1, Ryota Souzaki, MD, PhD2, Yo Kobayashi, PhD3, Masakatsu G Fujie, PhD3, Makoto Hashizume, MD, PhD, FACS1, Tomoaki Taguchi, MD, PhD, FACS1. 1Department of Pediatric Surgery, Faculty of Medicine, Kyushu University, 2Department of Advanced Medicine and Innovative Technology, Kyushu University Hospital, 3The faculty of science and engineering, Waseda University
BACKGROUND & AIM: In pediatric endosurgery, surgeons receive much benefit of magnified visual filed even for small body patients. On the other hand, the more visual filed was magnified, the more blind area of the forceps became bigger. In the previous study, we developed augmented reality (AR) navigation system and applied pediatric laparoscopic splenectomy (Ieiri S, et al., Pediatr Surg Int, 2012) and oncologic surgery (Souzaki R et al., J Ped Surg, 2013). Therefore we developed the blind area visualization system to resolve these demerits using AR technique for pediatric endosurgery. In this study, we verify an effectiveness of this system for pediatric surgeons.
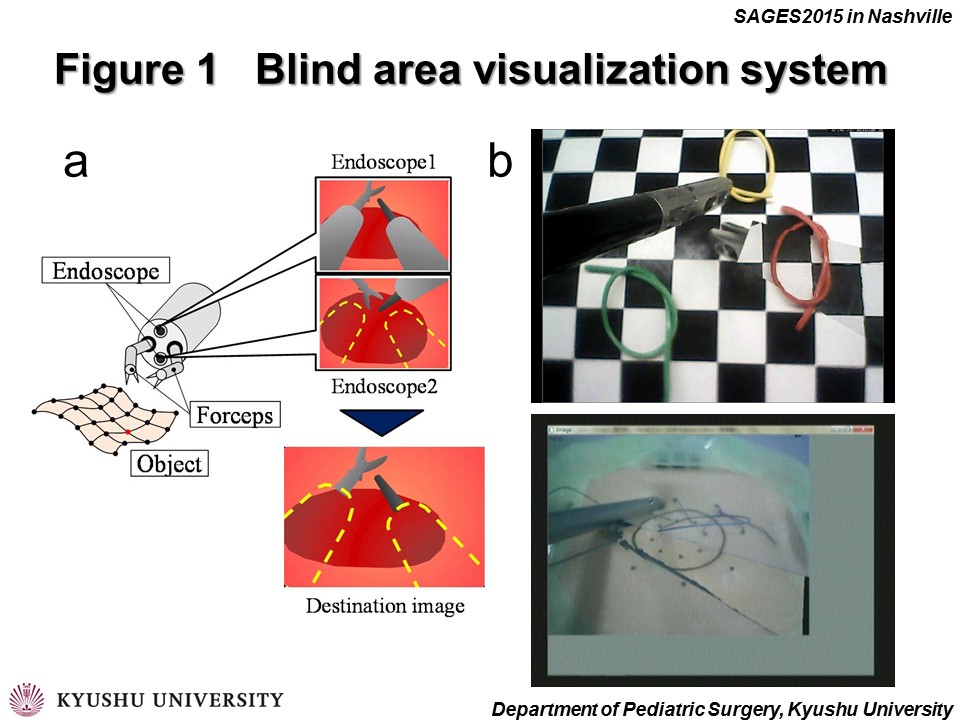
METHODS: Developed system was composed of two cameras. One is for usual view point of surgeon, and the other is for compensation of blind area of forceps. Image of blind area of forceps was fused with a real-time endoscopic image of the operative field, providing a transparent forceps for the surgeon (Fig.1a).Surgeons can get “See-Through Needle Driver” using this augmented reality technique (Fig.1b). We examined the effectiveness of this system by backhand needle driving (Fig.2). Examinees were 17 pediatric surgeons and they were divided into 2 groups, 3 experts and 14 trainees. They had to perform 3 backhand needle driving in the box without (Fig.2a) or with this system (Fig.2b). The tip of the needle was hidden by shaft of forceps. Such being the case, this task was setup. Evaluation points were time and accuracy. Accuracy was calculated by measuring of deviation of exertion error. Statistical analysis was performed Mann-Whitney U test and p<0.05 was considered statistically significant.
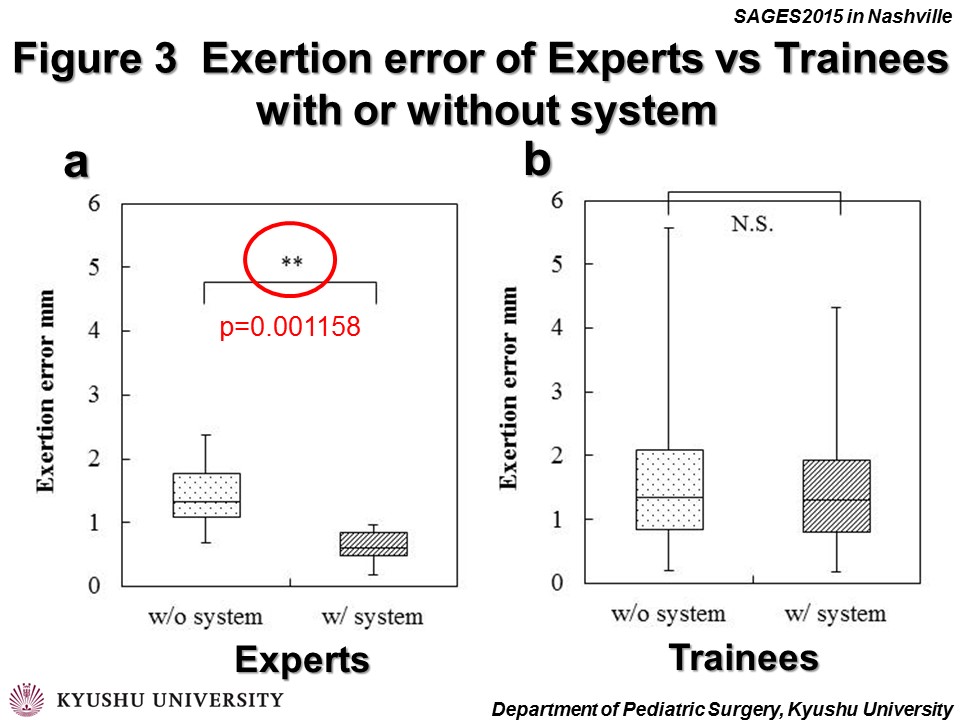
RESULTS: All 17 participants completed the evaluation task. There was no significant difference between with and without system for time, in experts and trainees, respectively. Figure 3 showed the results of needle driving accuracy. Exertion error of experts with and without system was 0.63 ± 0.43 and 1.40 ± 2.33 (p=0.001158) (Fig.3a), respectively. Exertion error of trainees with and without system was 0.63 ± 0.43 and 1.40 ± 2.33 (p=0.843972) (Fig.3b), respectively. Experts improved the backhand needle driving accuracy using this system.
CONCLUSIONS: The results revealed that the experts made skillful use “See-Through Needle Driver” using an AR technique. They would receive the maximum merit of this system for the magnified view of small working space. We can apply this technique all kinds of forceps, stapler, energy device and trocars. Next step, we must refine this system for in-vivo experiments. In the near future, this system would be applied for clinical use of advanced pediatric endosurgery, especially for small neonate and infant patients.