Introduction: It is known that feedback enhances the learning process, although the optimal type and frequency of feedback is not established. The ProMIS hand-assisted laparoscopic colectomy (HALC) simulator uses a combination of virtual reality (VR) and and physical models of intra-abdominal organs to simulate a left-sided hemicolectomy. It can be used to train surgeons to perform a complete procedure in a safe environment.
The purpose of this study was to determine if giving trainees feedback during a training session would improve their performance.
Methods: We tested 16 residents (Group 1) who performed 5 HALC procedures on the ProMIS simulator. Efficiency of instrument use and pre-defined intra operative error scores were assessed. Facilitators assisted their performance and answered questions when asked. A similar cohort of 12 trainee surgeons (Group 2) then performed the same 5 cases, but with standardized feedback and the chance to review errors after every procedure.Eight subjects in Group 2 completed retention testing which consisted of two further repetitions of the HALC procedure. Data were analyzed using SPSS version 15. Means were compared using Mann-Whitney-U tests, with a p-value of <0.05 taken as significant. Errors were analyzed by 2 blinded assessors.
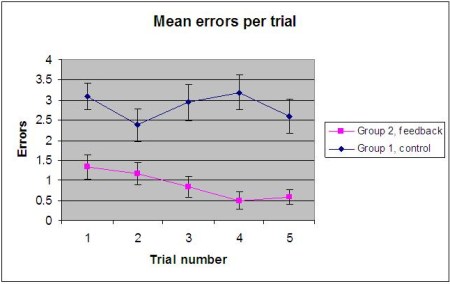
Results: Group 1 achieved better results for instrument path length (23,874mm vs 39,086mm, p= 0.001 overall, not significant (ns) on trials 1, 4) and instrument smoothness (2015 vs 2567, p = 0.045, ns on trials 1,2 and 4)). However, Group 2 (feedback) performed significantly better with regard to error scores (14 vs 4.42, p = 0.000, figure 1). In addition they demonstrated a smoother learning curve and their performance had reached a plateau by the fourth trial. Thepoorer instrument scores are likely a function of a more thorough dissection and error-free procedure.Inter-rater reliability for the error scores was 0.969. Eight subjects in Group 2 performed 2 cases each at a mean interval of 14.5 weeks after the initial training session. On average, their scores for instrument path length and smoothness deteriorated by 48% and 39% respectively compared to their performance on trial 5, but error scores deteriorated by only 0.05%.
Conclusion: In conclusion the provision of standardised proximate feedback was associated with significantly less errors and an improved learning curve. This occurred at the expense of instrument handling scores. Retention at 14.5 weeks was better for procedure –specific error scores than instrument handling scores. Reducing errors in the skills lab environment should lead toimproved clinical performance.The provision of structured feedbackmay therefore help to make training more efficient and improve patient safety.
Figure 1 – mean error scores per trial for group 1 and group 2
Session: Podium Presentation
Program Number: S098