Elijah Kim, MD, MPH, FACS, FCCP, Patrick Collier, MD, Corydon Siffring, MD, FACS, Erin Hagerman, MSN, AGACNP, Tina Molohon, TPC, RN, TNS, Douglas C Maibenco, MD, PhD, FACS. HSHS Medical Group Trauma/Acute Care Surgery, St. John’s Hospital, Springfield, Illinois
Introduction: Robotic distal pancreatectomy for trauma has never been reported. We present a case of blunt abdominal trauma resulting in a Grade III injury of the pancreatic body with complete transection at the confluence of the inferior mesenteric and splenic veins. The patient was taken emergently to the operating room where a robotic assisted spleen preserving distal pancreatectomy was performed. We describe the patient selection, technical details, and postoperative course, as well as indications, contraindications, and implementation of robotic assisted surgery for trauma to the pancreas.
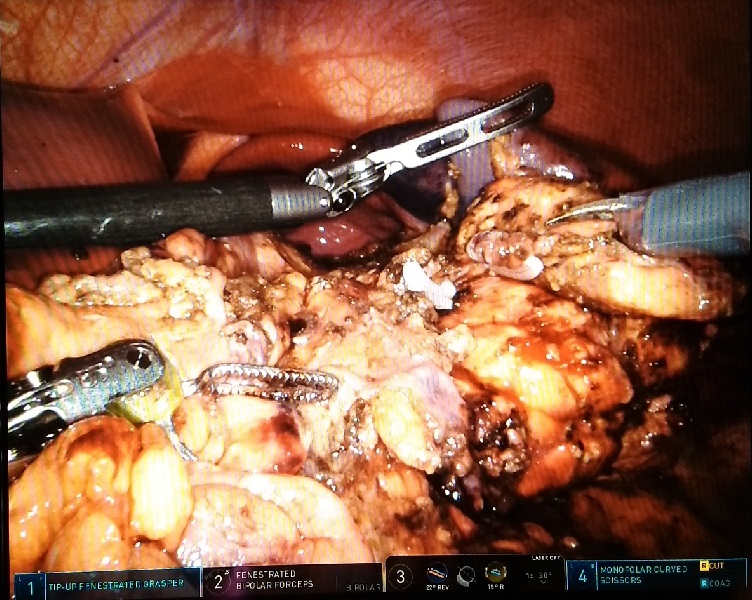
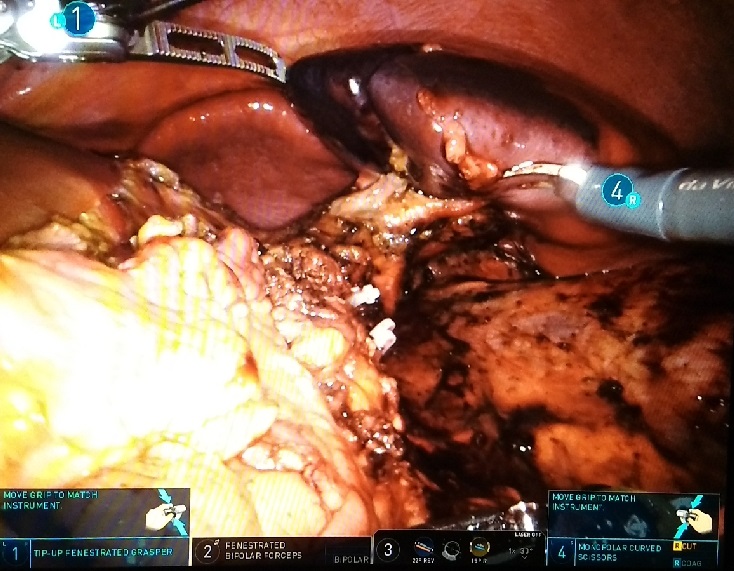
Methods and Procedures: The patient is an 18-year-old male who sustained a football injury to the left upper quadrant and presented hemodynamically stable. Computed tomography demonstrated a Grade III pancreatic injury. With the patient in right lateral decubitus position, one 12mm and three 8mm robotic trocars were used to gain entry. Inspection verified the pancreatic body to be transected. Venous bleeding was controlled and no active arterial bleeding was noted. The splenic vessels and the inferior mesenteric vein were identified and preserved. The proximal pancreatic body was closed using 2.5mm staples, fibrin glue, hemostatic agent, and an omental buttress. The distal pancreas was morselized and retrieved via the 12mm trocar site resulting in the loss of approximately 40% of pancreatic volume. Estimated blood loss was 100mL. Total operative time was 346 minutes.
Results: Postoperatively, the patient was treated with total parenteral nutrition and octreotide. A left pleural effusion was drained under ultrasound guidance on day six. Enteral feeds were started on day six via a nasojejunal feeding tube. Abdominal drain output diminished significantly by day eleven. He was started on an oral diet and discharged home. Total length of stay was 13 days.
Conclusion: Although initially developed with remote trauma surgery in mind, robotic assisted surgery is currently utilized nearly exclusively for elective surgery. Search in the current literature demonstrates a noticeable absence of robotically assisted surgery for trauma. With appropriate patient selection, experienced trauma surgeons comfortable with robotic and open techniques, and hospitals prepared and equipped with sufficient capacity, regional trauma centers can safely provide minimally invasive robotic surgery for trauma and take full advantage of the modality including potentially minimizing pain, large incisions, blood loss, conversion rates to open, splenectomy rates, and length of stay. Ongoing progress in the adoption of robotic assisted trauma surgery is helping to realize some of the intentions that inspired the original developers of the technology.


Presented at the SAGES 2017 Annual Meeting in Houston, TX.
Abstract ID: 92273
Program Number: P654
Presentation Session: Poster Session (Non CME)
Presentation Type: Poster
