Matthew Y Lin, MD, Ankit Sarin, MD MPH, M. Mehdi Tavakol, MD, Shadee M Amirkiai, BS, Stanley J Rogers, MD, Jonathan T Carter, MD, Andrew M Posselt, MD PhD. Department of Surgery, University of California, San Francisco, School of Medicine, San Francisco, California
Abstract
Background: Obesity, steroid-induced diabetes, hypercholesterolemia, and steatohepatitis can occur after liver transplantation and may respond to bariatric surgery. The safety and feasibility of bariatric surgery after liver transplantation is unknown.
Methods: Nine morbidly obese patients with prior liver transplants underwent sleeve gastrectomies in a pilot program. Sleeve gastrectomy was chosen over gastric banding to avoid foreign body implantation, and over gastric bypass to maintain endoscopic access to the biliary system and reduce surgical complexity. We reviewed patient demographics, operative details, 30-day complications, weight loss, postoperative hepatic and renal function, and resolution of co-morbidities.
Results: Patient and procedural characteristics are listed in Table 1. The operation was performed laparoscopically in 8 patients and open in one patient. Follow-up ranged 3-36 months. Excess weight loss averaged 55.5% at 6 months (table 2). Calcineurin inhibitor levels, hepatic, and renal functions remained stable. There were no episodes of acute rejection. In the first 30 days, there were 3 complications: mesh dehiscence after a synchronous incisional hernia repair, bile leak from the liver surface that resolved with conservative management, and postoperative dysphagia with readmission.
Table 1. Demographics and Laboratory Values
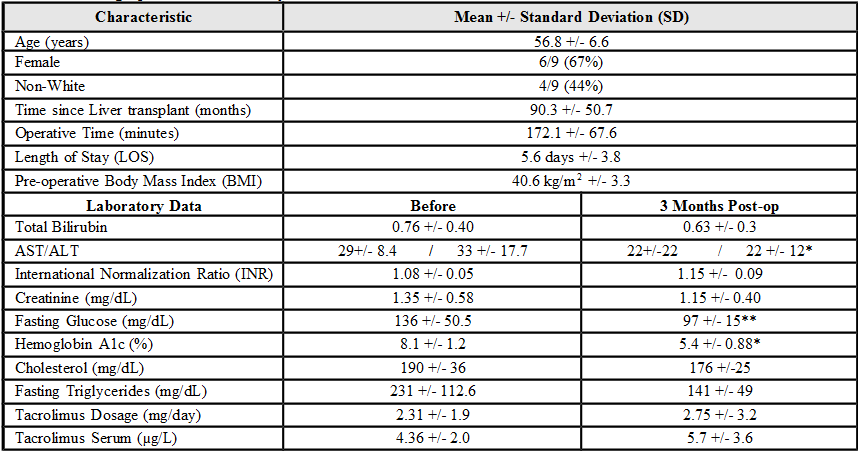
Table 2. Weight Loss
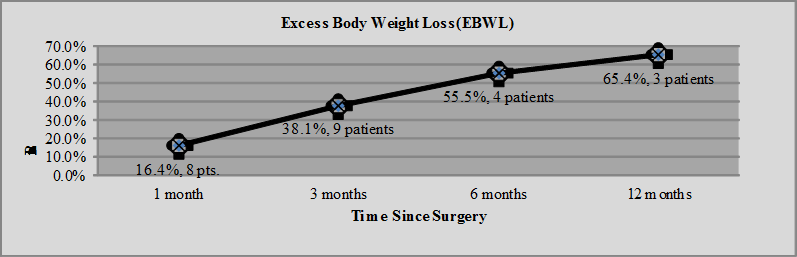
Conclusion: Sleeve gastrectomy is technically feasible after liver transplantation and results in weight loss and improvement in metabolic diseases. Graft function and immunosuppression are not adversely affected. Complications might be more frequent given the patient’s underlying disease and prior surgeries.
Session Number: SS09 – Obesity Surgery
Program Number: S060
