James Bittner, MD, Debra Tiemann, RN, Angelia Declue, Michael M Awad, MD PhD. Washington University in St. Louis School of Medicine
INTRODUCTION
In this era of proficiency-based training and limited duty hours, the role of simulation in medical education is becoming increasingly important. However, virtual reality (VR) simulators are often out of reach for most education centers because of their expense. In this study, we sought to compare the utility of a high-fidelity VR colonoscopy simulator to that of a low-fidelity plastic simulator and colonoscope received as part of the SAGES/Olympus Surgeons Training Endoscopic Proficiency (STEP) program.
METHODS
From 2009-2011, 35 PGY-2 and -3 surgical residents participated in two-hour endoscopy training sessions, during which they performed simulated colonoscopy, then completed their formal endoscopy rotation. The objectives of the session were to learn (1) basic scope operation, (2) scope setup and troubleshooting, (3) scope navigation, (4) visualization of colonic mucosa, and (5) endoscopic biopsy. Residents trained for one hour each using a VR colonoscopy simulator (~$20,000; Immersion Medical, Inc.) and the STEP colonoscope (CF-H160, Olympus America, Inc.). For the VR simulator, trainees performed the basic scope navigation, advanced scope navigation, and biopsy modules. For the STEP simulator, trainees were first given instruction regarding assembling and disassembling the scope/tower and then were asked to navigate through a custom-developed simulator made of hamster tubing based on a model from Southern Illinois University ($57.80). Within this model are numbered stickers, a pool of fluid for suctioning, and a simulated sessile polyp made of putty. After the training session, residents completed a survey rating the extent to which the five stated objectives were accomplished by each of the simulators (1=Strongly disagree, 5=Strongly Agree). At the conclusion of the four-week endoscopy rotation, trainees once again were asked to complete the same survey. Student’s t-test was used to compare survey responses between training groups (α=.05).
RESULTS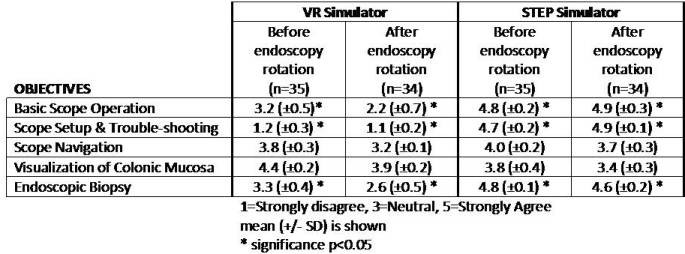
CONCLUSIONS
Trainees perceived the STEP simulator to be equivalent or better than the more expensive VR simulator for all five training objectives. The differences were particularly pronounced for the basic scope operation, scope setup/troubleshooting, and biopsy objectives. These were objectives for which having an actual scope, similar to that used during the endoscopy rotation, was perceived as most beneficial. The STEP program may enable training programs to achieve their stated goals for basic diagnostic colonoscopy training with low-cost alternatives to expensive commercial simulators.
Session Number: Poster – Poster Presentations
Program Number: P174
View Poster
