Kryztopher D Tung, MS, Rami M Shorti, MS, Earl C Downey, MD, Donald S Bloswick, PhD, Andrew S Merryweather, PhD. Mechanical Engineering Dept., University of Utah, Salt Lake City, UT, USA.
Introduction: A multitude of factors can affect a surgeon’s performance in the operating room; these may include surgeon comfort and skill level, tool handle ergonomics, and fatigue. The goal of this study is to quantify the effects of ergonomic laparoscopic tool handle design on surgeon performance and task completion efficiency. A laparoscopic tool handle designed with ergonomic considerations (pistol-grip) was tested against a current market tool with a traditional (pinch-grip) handle.We hypothesized that there will be a measurable difference between the efficiency of FLS surgical trainer tasks of the pistol-grip versus the pinch-grip laparoscopic tool handle designs in three categories: time to completion, technical skill, and subjective user ratings.
Methods and Procedures: The pistol-grip incorporates an ergonomic interface intended to promote a more neutral operating posture, and influence the degree of hand tremor and fatigue while reducing contact stress points on the hand and fingers. The pinch-grip is a widely used current market tool. Twenty-three (13 M, 10 F) naïve participants (medical students) with no existing upper extremity musculoskeletal disorders were selected for this study. During a training session prior to testing, participants performed practice trials in a SAGES FLS trainer with both tools. During data collection, participants performed three evaluation tasks with each tool. These consisted of a peg transfer task, a cutting task, and a suturing task. Two participants (1M, 1F) were excluded from the final analysis due to incomplete or missing data.
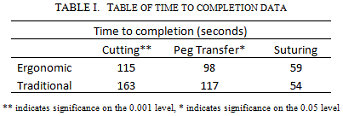
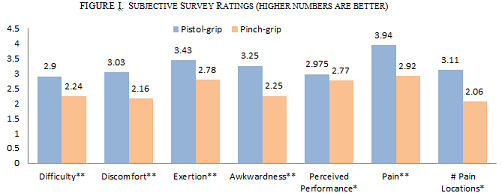
Results: Quantified survey feedback (Figure 1) from test participants significantly favors the pistol-grip in every category (P<0.05). While there was no significant interaction between tool type and errors (P>0.7) made during trials, time to trial completion was significantly lower for the pistol-grip tool during cutting (P=0.001) and peg transfer (P=0.007) tasks (Table 1). While there was no difference for the suturing task (P=0.586), it is important to note that the needle grasper was the same for both tools and was used in the dominant hand.
Conclusions: These findings favor the pistol-grip design and are part of a much larger study to quantify the effect of laparoscopic tool handle design on upper extremity biomechanics. Further testing with professionally trained laparoscopic surgeons in a more realistic test environment is needed to evaluate performance metrics including contact stress, posture, muscle fatigue, and economy of movement.