Mark R Wendling, MD, James D Vargo, Joseph M Drosdeck, MD, W. Scott Melvin, MD, Vimal K Narula, MD
The Ohio State University Wexner Medical Center
Objective
Bile duct injury remains the most feared complication of laparoscopic cholecystectomy. Intra-operative Cholangiography (IOC) is currently the gold standard for biliary imaging, but technical challenges and time requirements limit its use. We aim to establish Near Infrared Fluorescence Cholangiography (NIRF-C) as an effective, reliable method for identifying pertinent biliary anatomy during laparoscopic cholecystectomy to provide surgeons with an efficient method of real-time biliary imaging.
Description/Methods
NIRF-C is a non-invasive method of real-time, radiation free, intra-operative biliary mapping. Pre-operatively, a fluorescent dye, indocyanine green (ICG), is administered intravenously. Bound to plasma proteins, ICG is taken up by hepatocytes and excreted, unaltered, in bile within 20 minutes. A laser on the laparoscope excites ICG in the biliary tree eliciting near infrared fluorescence (~800 nm) which is captured by an image filter on the laparoscope. Surgeons may toggle between NIRF-C and the standard view on the laparoscope.
Eighty-two patients will undergo intra-operative biliary mapping with both NIRF-C and IOC. Two-and-a-half milligrams of ICG is administered intravenously 30-60 minutes prior to the procedure. NIRF-C is used to identify extrahepatic bile ducts before dissection, after initial dissection, and after final dissection. IOC is performed after final dissection and all data regarding NIRF-C has been recorded. During both techniques, data regarding the successful identification of the following structures is collected: right and left hepatic ducts, common hepatic duct, cystic duct, cystic/common hepatic duct junction, common bile duct (CBD), cystic artery, and anatomic variants. Length of procedure, complications, and time required to complete NIRF-C and IOC are also recorded.
Preliminary Results
Five patients underwent laparoscopic cholecystectomy with NIRF-C and IOC for symptomatic cholelithiasis, biliary colic, or chronic cholecystitis without complications. All patients were female with a mean age of 37.6 (28-60) and BMI of 26.7 (19.8-31.1). Mean time from ICG administration to incision was 61.2 min (40-91). Mean operative time was 74.4 min (48-137). Surgeons spent 44% less time on NIRF-C than IOC: average time spent on NIRF-C was 6 min (1.62-10.58), compared to 10.66 min for IOC (7.33-13.75) (Table 1).
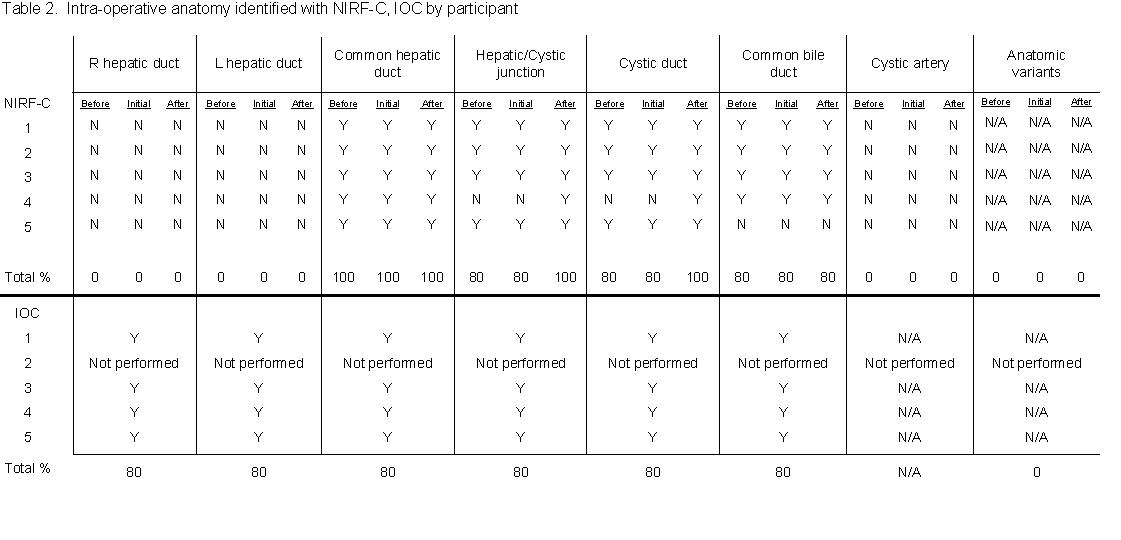
NIRF-C identified over 80% of extrahepatic biliary anatomy during laparoscopic cholecystectomy. In all cases, the common hepatic duct was visualized before dissection. The incidence of cystic duct and cystic/hepatic duct junction visualization was 80% prior to dissection and 100% after final dissection. The incidence of CBD identification was 80% prior to dissection. In one case the CBD was not visualized after final dissection. IOC identified all biliary structures in 80% of cases. In one case, it was aborted due to technical difficulties (Table 2).
Conclusions/Future Directions
Preliminary data reveal that NIRF-C is non-inferior to IOC in successfully imaging extrahepatic biliary structures when use-limiting technical challenges of IOC are considered. Additionally, NIRF-C requires less time than IOC and is performed with fewer logistical barriers. These attributes affirm NIRF-C as a promising new method for routine cholangiography, potentially supplanting the need for IOC. Thus far, NIRF-C appears to be a safe, effective, and efficient method for identifying extrahepatic biliary anatomy during laparoscopic cholecystectomy.
Session: Podium Presentation
Program Number: ET002
.JPG)